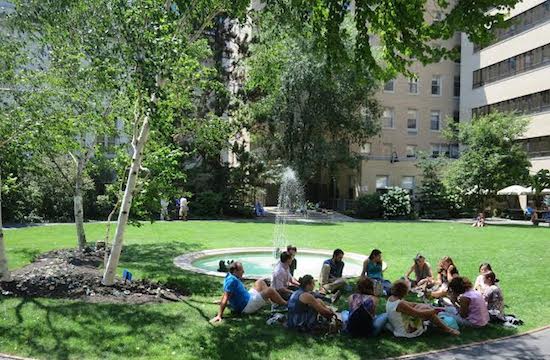Connecting kids with heart disease and horses
At Windrush Farm
Edited from a New England Council report (newenglandcouncil.com)
“Boston Children’s Hospital (BCH), in its treatment of patients with complex congenital heart disease, is connecting young children with horses to bolster their emotional and physical strength. The New England Council member has seen success with the unique program.
“Since 2017, BCH has partnered with Windrush Farm, in North Andover, Mass., to offer equine-assisted therapy to patients. The children have the opportunity to bond with and ride a horse, receiving the fulfillment of accomplishment. Additionally, patients receive many physical benefits, as riding trains their balance, strength, and flexibility. For these children who have battled with this disease since birth, there is great value in experiencing the confidence, assertiveness, and collaboration required in riding horses. Furthermore, the animals offer an emotional outlet, where patients can release the anxiety and stress that develops after a childhood affected by the disease.
“‘For kids who haven’t felt successful in much of their lives, this helps them build independence, confidence, and self-esteem,’ said Kate Ullman-Shade, the director of education for the cardiac neuro-developmental program at BCH. ‘I’ve had kids say to me, ‘I’m so proud of myself.’”’
Boston Children’s to buy Franciscan in bid to improve mental-health care
Boston Children’s Hospital
Via The New England Council (newenglandcouncil.com)
“Boston Children’s Hospital plans to acquire Franciscan Children’s {hospital}, in Boston’s Brighton section. Through this acquisition, Boston Children’s Hospital hopes to improve its response time for children who are awaiting psychiatric treatment and expand the mental-health resources available to its patients.
“As the coronavirus pandemic persists, there has been a significant uptick in the number of patients receiving or waiting for inpatient psychiatric care at Boston Children’s Hospital. By joining forces, Boston Children’s Hospital can increase and diversify its mental-health resources offered to patients, expanding into services such as treatments for those with psychiatric disorders and developmental disorders. This acquisition would also allow for Boston Children’s hospital to better manage the increase in patients who seek treatment.
“Dr. James Mandell, chairman of the Franciscan Children’s board, recognizes that this plan would be mutually beneficial, as the acquisition would provide Franciscan Children’s with the opportunity to ‘better train and recruit staff,’ and ‘provide access to more patients.’’’
Children's Hospital to study COVID-19 mystery; Assumption College holds to plan to train PA’s
Boston Children’s Hospital
From The New England Council (newenglandcouncil.com):
As our region and our nation continue to grapple with the Coronavirus Disease (COVID-19) pandemic, The New England Council is using our blog as a platform to highlight some of the incredible work our members have undertaken to respond to the outbreak. Each day, we’ll post a round-up of updates on some of the initiatives underway among Council members throughout the region. We are also sharing these updates via our social media, and encourage our members to share with us any information on their efforts so that we can be sure to include them in these daily round-ups.
You can find all the Council’s information and resources related to the crisis in the special COVID-19 section of our Web site. This includes our COVID-19 Virtual Events Calendar, which provides information on upcoming COVID-19 Congressional town halls and webinars presented by NEC members, as well as our newly-released Federal Agency COVID-19 Guidance for Businesses page.
Here is the April 29 roundup:
Medical Response
Boston Children’s Hospital Launches Study on COVID-19 in Pediatric Patients – To better understand why few children infected with COVID-19 become severely ill, Boston Children’s Hospital has initiated a national study of 800 infected children. The study will examine patients with varying levels of symptoms to identify what protects children from severe symptoms that older patients lack. WBUR has more.
Blue Cross Blue Shield of Massachusetts Deploys 100 Employees to Support Boston Response – Blue Cross Blue Shield of Massachusetts (BCBSMA) is re-assigning 100 of its employees to aid Boston’s response to the pandemic. Workers from BCBSMA will support the city’s contact tracing efforts and care efforts at Boston Hope field hospital. Read the press release here.
Massachusetts General Hospital Partners with Boston to Identify Asymptomatic Residents – Massachusetts General Hospital (MGH) and the City of Boston have partnered to launch new initiative to evaluate community exposure to COVID-19 using antibody testing and. MGH and the city will randomly select residents in the hardest-hit parts of Boston to guide future allocation of resources. Read more from WBUR
Economic/Business Continuity Response
Assumption College Continues Developing Physician Assistant Program – Despite the pandemic suspending most plans, Assumption College is moving forward with its new physician assistant program. Leaders of the new program are hoping the outbreak can even inform the new program’s focus on care during a pandemic. The school is still planning to enroll students in January 2021 while awaiting accreditation and building clinical partnerships. Read more in MassLive.
Partners HealthCare Requires Rapid COVID-19 Testing on Admission in Hospitals – At all of its acute care hospitals, Partners HealthCare is requiring all admitted patients to undergo a COVID-19 test. The new regulation is designed to gather data about the spread of the virus within the provider’s facilities to inform decisions surrounding protective equipment orders and floor layouts—as well as to protect patients and staff. Read more from WBUR.
Community Response
Tufts Health Plan Announces $345,000 in Funding for Relief Efforts – As part of its commitment to support relief measures targeting older people, Tufts Health Plan has pledged $345,000 to organizations focusing on housing insecurity in New England. The organization is also accelerating payments to current community partners and matching employee donations, raising an additional $55,000 for the organizations. Read more.
Holy Cross Uses Day of Giving Funds to Support Students Affected by Pandemic – The annual day of giving at the College of the Holy Cross raised $2.47 million to support current students and staff at the school. The school community prioritized donations to causes—such as its Emergency Relief Fund to offset short-term costs for unanticipated technology, housing, and travel costs for students—that will support those at the school most significantly impacted by the pandemic. Read more here.
Stay tuned for more updates each day, and follow us on Twitter for more frequent updates on how Council members are contributing to the response to this global health crisis.
View of the entry to Assumption College and of the Blessed Virgin from the La Maison building
3 Boston hospitals partner to help low-income families with rent
The Boston Medical Center’s Moakley Building
This is from The New England Council (newenglandcouncil.com):
BOSTON
“New England Council members Boston Children’s Hospital and Brigham & Women’s Hospital have partnered with Boston Medical Center (BMC) to launch a program to aid families struggling with rent. By joining forces on this initiative, the three major Boston hospitals are recognizing a substantive connection between stable housing and good health.
“Research conducted by BMC has shown that housing, alongside food and education, plays a critical role in an individual’s health and their health care costs. Children are especially vulnerable to health issues and developmental delays if they lack a stable housing situation. City officials found than over 4,600 eviction cases were filed in Boston Housing Court in 2016, the majority of which involved residents in subsidized housing. As rent continues to rise in Boston, the hospitals identified access to affordable, stable housing as a major concern for low income families and their health.
“The three hospitals plan to donate over $3 million over three years to fund housing programs and community grants. The first $1.5 million has be reserved for families behind on rent and at risk for eviction. Because of the hospitals’ financial commitment to this project, all three have also been granted state approval for construction plans at each of their campuses.
“‘The hospitals don’t think they’re going to fix the housing problem,’ said Dr. Shari Nethersole, executive director for community health at Boston’s Children’s. ‘We recognize this is a societal problem. We’re trying to help identify where we do have a role, where we can help.’
“The New England Council commends all three institutions for their commitment to support the health of low- income families.
Melissa Bailey: Bringing home dying children
Boston Children’s Hospital
From Kaiser Health News
Anne Brescia sat beside her only child, Anthony, as he lay unconscious in a hospital bed at age 16. Just a few months before, he was competing in a swim meet; now cancer was destroying his brain. Brescia couldn’t save her son. But she was determined to bring him home.
Anthony Gabriel Brescia-Connell was not conscious for his voyage from Boston Children’s Hospital to his home in Medford, Mass., where he died on March 3, 2011, surrounded by his family and beloved stuffed animals. He may not have heard the parting blessings before a doctor turned off his portable ventilator and let him die naturally.
But having the choice to take Anthony home, away from the beeping hospital monitors, “meant the world to me,” his mother said.
Anthony’s journey was made possible through swift and unconventional efforts by the hospital staff, including a critical-care transport team accustomed to rushing kids to the hospital to save their lives, not taking them home to die.
The experience galvanized Harriett Nelson, a nurse on that team who helped arrange the trip. It inspired her to conduct pioneering research on and advocate for “pediatric palliative transport” — a rare but growing practice that aims to give families choice, control and comfort at the end of life.
Palliative transport lets families move critically ill children from the hospital intensive care unit to their home or hospice, with the expectation they will die within minutes to days after removing life support.
It means “having parents go through the hardest thing they’ll ever know — in the way they want to do it,” Nelson said. Boston Children’s has sent 19 children to home or hospice through palliative transport since 2007, she said.
These final journeys — also offered by Mayo Clinic, Children’s Hospital of Philadelphia and Kentucky Children’s Hospital — can involve elaborate planning, delicate transfers and even long helicopter rides. In some cases, families took a child far from home for a last-ditch effort to save their lives.
At Mayo Clinic, in Rochester, Minn., palliative transport has helped culturally diverse families carry out end-of-life wishes for their dying children. In one case, a newborn girl rode 400 miles by ambulance to return to her Amish community, where she was extubated and died in her parents’ arms, in the company of her 11 siblings. In another, an 8-month-old Native American girl traveled 600 miles by air and ground ambulance to her rural tribal reservation, where she could participate in end-of-life rituals that could not be done in the hospital.
These trips, which can cost thousands of dollars, are typically offered free to families, paid for by hospitals or charities. Most children are taken home, where they transition to receiving care from hospice staff. Some go instead to hospice facilities.
Dr. Megan Thorvilson, a pediatrician and palliative care specialist at Mayo Clinic, said palliative transport aims to address a gap between families’ preference and reality. Most parents of terminally ill children would prefer that their child die at home, but most of these children die in the hospital, most commonly in the intensive care unit. Most pediatric ICU deaths happen in a controlled way, following the removal of life support, she noted. That means there may be time to move the child to an alternative location to honor a family’s wishes.
Transporting children on life support is risky. At a palliative care conference, a nurse from Children’s Hospital of Philadelphia described the difficulties staff faced in trying to fly a 10-year-old girl home to Michigan. After she was rolled on her side several times to be transferred between vehicles, the child died before the plane could take off.
And dying at home is not what every family wants.
“We do sometimes overly romanticize the death at home,” Thorvilson acknowledged. Some parents would much rather have a child die in the hospital, with familiar nurses at the bedside for medical and emotional support. Some would rather keep this traumatic experience away from where they live.
Brescia, however, said she couldn’t bear to return home without her son.
Brescia, a biologist who used to run an electron microscopy lab, wasn’t sure if she and her husband, Brian Connell, would ever have kids. Fertility treatments didn’t work. But on June 23, 1994, seven days before Brescia turned 44, she gave birth to a baby boy.
“Anthony is the love of my life,” said Brescia, who is now 68. “The OB-GYN put him on my chest and I really thought that my heart was going to burst.”
The mother-son bond was especially close: Brescia home-schooled her son for most of his life. Anthony grew to be 6 feet tall, full of curiosity. He loved identifying mushrooms, studied Arabic and oceanography, and aspired to go to MIT. He was an avid swimmer, competing on a team in Belmont, Mass.
One day in late 2010, while racing the backstroke, he became disoriented in the pool and was disqualified.
A neurologist prescribed rest. But over the next two weeks, Anthony grew only more tired and began to lose his balance. On Dec. 20, he was taken to Boston Children’s Hospital and diagnosed with a brain tumor.
The disease “came out of nowhere,” Brescia recalled. “He went from looking incredibly healthy and swimming like a healthy kid” to living at the hospital. At his bedside, she told him she’d bring him home to celebrate Christmas and eat stuffed shells.
His condition deteriorated very quickly. The tumor could not be surgically removed. Anthony pushed through radiation and chemotherapy with the hope of going home, but the treatments failed. By late February 2011, the tumor began pressing on his brain stem, and fluid was building up in his brain.
Anthony was unconscious, relying on a ventilator to breathe. Brescia connected with the hospital’s palliative care team.
“I want to bring him home tomorrow,” Brescia told the staff.
“I was scared to death he was going to have another incident,” she recalled. “I didn’t want them to do any more invasive procedures to reduce the pressure on his brain.”
Staff from the ICU, palliative care and transport teams scrambled to honor her request. The critical care transport team arranged for the use of its ambulance, a mobile ICU the size of a small bus.
The night before the trip, Brescia said goodbye in the privacy of Anthony’s hospital room.
“I don’t want to lose you,” she told him, holding his hands. “I’m going to let go. I want you to go where you need to be.”
On March 3, 2011, Brescia and her husband boarded the bus along with Anthony, a chaplain, two doctors, Nelson and a nurse from the ICU. They rode 10 miles to the family’s home, where Anthony was laid on a hospital bed in his living room, surrounded by his stuffed animals, on his favorite flannel sheets.
A pastor held a service for Anthony, and close family gathered to say goodbye. Then Brescia signaled for a doctor to disconnect the ventilator.
Anthony seemed to be at peace, Brescia said. After he died, she climbed into the bed with her son and held onto him for a while.
The death was still traumatic. But “it was really a gift to bring him home,” she said. “It was a significant act of compassion and kindness and love on the part of the Children’s staff.”
After Brescia’s experience, Nelson was inspired to offer the choice to more families. First, she interviewed Brescia and other parents about whether palliative transport had had a positive impact. All nine parents said it had. One family described holding a celebration when they brought their newborn baby home, even though he was about to die. They took family photos and used the nursery they had set up, establishing a brief sense of normalcy for four days before he died.
In her 14 years on Boston Children’s critical transport team, Nelson has found that parents benefit from palliative transport for various reasons: At home, they’re away from the noise of the hospital. They have control over who can visit. They feel more comfortable. And they don’t feel rushed after their child dies.
Nelson created a protocol that allows the hospital to offer palliative transport in a more routine way. Now, when children come to any of the hospital’s four ICUs, Nelson said, “we have the power to say, ‘You have a choice when it comes to the end of life.'”
The practice appears to be spreading.
After Dr. Lindsay Ragsdale, director of the palliative care team at Kentucky Children’s Hospita,l in Lexington, presented her protocol for palliative transport at a conference last year, staff from 20 hospitals asked her to share her checklist, she said.
Mayo’s Thorvilson, who has worked closely on a half-dozen palliative transports, said it’s possible these last-minute trips from ICU to home could be avoided by earlier referrals to hospice, which might get kids home sooner. But when children with complex illnesses get sick, she said, “sometimes it’s hard to know whether this is just another bump in the road, or whether this is the natural end of the child’s life.”
“There’s something really unique about a child dying,” she said. “Everyone’s heart breaks, and we want to be able to do all that we can to be able to support the family in the midst of the tragedy.”
Eight years after Anthony’s death, his bedroom remains unchanged. (KAYANA SZYMCZAK FOR KHN)
Eight years after Anthony’s death, his bedroom remains untouched, his socks still folded in his top drawer, swimming trophies on the cabinet, slippers under his chair. Pictures of him adorn every room in the house — on the fridge, the kitchen table, the living room stereo.
Looking through photos one recent morning of her son fishing and blowing out birthday candles, Brescia struggled to hold back tears.
“I couldn’t cure him,” she said. “I failed to protect him from a tumor — that’s how you feel. They did all they could. It wasn’t enough. Bringing him home was the best I could do.”
Melissa Bailey: mbailey@kff.org, @mmbaily
Boston Children's Hospital partners with 2 R.I. hospitals
From The New England Council (newenglandcouncil.com)
Boston Children’s Hospital has announced an alliance with two of the region’s top hospitals in an effort to improve treatment for children diagnosed with complex conditions or behavioral health issues. By partnering with Hasbro Children’s Hospital and Bradley Hospital—both in Providence– the process will be streamlined for seriously ill children who need treatments or surgeries that are not offered at all the hospitals.
This new partnership will make it easier for patients at Hasbro Children’s Hospital to see doctors who specialize in stem cell transplants at Boston Children’s Hospital, while allowing that hospital’s patients to access fetal surgeries that are not done at Boston Children’s. The inclusion of Bradley Hospital, which is the nation’s first psychiatric hospital just for children, will round out specialized care options of kids by including mental health.
Sandra L. Fenwick, CEO of Boston Children’s Hospital, said, “This agreement recognizes that great care should be provided as close to a patient’s home as possible, which can be achieved only if we work with other excellent pediatric hospitals. Boston Children’s and Hasbro Children’s together have the determination and know-how to bring the best quality outcomes to patients efficiently.”
Boston Children's Hospital again ranked first
This is from the New England Council (newenglandcouncil.com)
"Boston Children’s Hospital was recently ranked first for the fifth straight year in the U.S. News and Report’s 12th annual list of best children’s hospitals. The rankings are based on metrics like patient outcomes, patient safety, number of fellowship programs, nurse-to-patient ratio, and availability of specialists and advanced services.
Boston Children’s Hospital ranked first in three of the ten specialties: neurology/neurosurgery, nephrology, and orthopedics. Additionally, the hospital placed second in cardiology and heart surgery, diabetes and endocrinology, and gastroenterology (GI) and GI surgery.
Boston Children’s President and CEO Sandra L. Fenwick said, “In a time when health care is ever-changing, achieving the number one ranking reminds all of us at Boston Children’s what inspires us: it’s about caring for children, digging deeper research, and finding new ways to make our care even better.”
Boston Children's Hospitals makes big advance against diabetes
This from the New England Council (newenglandcouncil.com):
"Boston Children’s Hospital recently cured type 1 diabetes in mice, bringing them one step closer to finding a cure for the disease in humans. cured type 1 diabetes in mice, bringing them one step closer to finding a cure for the disease in humans.
Researchers at the hospital have been working with mice on an immunotherapy treatment that replaces a genetic defect in blood stem cells with the patient’s own blood cells. The hospital discovered a genetic defect that decreases the PD-L1 protein therefore weakening the patient’s immune system and causing the disease. The mice that were infused with their own blood cells were all cured in the short-term and one third of the mice were cured for the rest of their lives. In initial human trials, the treatment met all FDA requirements and found no adverse effects, but more research is required to establish the ideal frequency of the treatment. Boston Children’s is currently working with Fate Therapeutics to optimize the treatment.
“We think resolution of (this problematic gene) may provide a novel therapeutic tool for the disease,” said Moufida Ben Nasr, a leading researcher with Boston Children’s Hospital.''
Thomas M. Paine: Save Boston Children's Hospital's healing garden
The Prouty Garden, at Boston Children's Hospital.
-- photo by Thomas M. Paine
For almost 60 years Boston Children’s Hospital considered the acclaimed Prouty Garden an integral part of its mission. The garden’s donor, longtime hospital trustee Olive Higgins Prouty, who had lost two young daughters, had the word of then-President William Wolbach that the garden she was endowing in 1956 would remain forever. That commitment is about to end unless the board quickly rethinks its plan to demolish the garden in a proposed $1.2 billion project to overhaul the hospital’s neonatal intensive-care unit and replace 82 semi-private rooms with single rooms with showers and clothing storage.
From its creation, Prouty Garden has been a sanctuary of healing where children confined for long periods can brighten their stays and hasten their recovery with daily visits to smell the flowers, discover the hidden statues, or see themselves reflected in the fountain pool. The expansive lawns, majestic dawn redwood, shrubs and perennial borders have provided respite for countless distraught families, visitors and overworked hospital personnel. Many children have spent their last moments on earth in the peace of Prouty Garden. It is where President John F. Kennedy came to grieve after the loss of his newborn son, Patrick Bouvier Kennedy. Originally designed by the famed Olmsted Brothers firm, Prouty Garden is “one of the most successful hospital gardens in the country,” according to healing-gardens authority Clare Cooper Marcus.
Prouty Garden advocates maintain that, frustrated with delay and wary of ballooning costs, the board has rejected some 17 plans that would preserve Prouty Garden. All 17 apparently had “fatal flaws.” The chosen plan was the only one considered that sacrifices Prouty Garden. Such decisions are never easy, and precisely what factors informed the decision process are not public. The board apparently, and no doubt reluctantly, concluded that Prouty Garden is not an inviolable part of the hospital’s mission but rather a temporary, expendable amenity.
To compensate for the loss, the selected design includes other landscaping. The renderings available online show a ground-level courtyard crisscrossed by walkways separated by raised planters of bamboos underplanted with groundcover. There are pocket parks in upper floors of the 11-story building, and a green roof. But does that settle the matter?
The fragmented greenspace in the preferred plan cannot compare with the expansive 23,000-square-foot Prouty Garden, with its spacious lawn under open skies, on firm ground, away from busy walkways, where kids can roam and families can find solitude. Even the largest green space in the design, the proposed outdoor courtyard, offers none of that immersive power, and the small pocket gardens on the upper levels can do even less. A green roof would hardly offer calm and security, let alone be planted with large trees or be visible from a hospital window. As to where families would go to grieve alone, or terminally ill children would spend their last moments, the proposed spaces are no substitute for Prouty Garden.
Board members have rightly emphasized the needs of the children over the needs of the hospital. But have they adequately considered how the garden itself serves children’s needs? Environmental psychologist Roger Ulrich demonstrates that experiencing nature in a hospital garden even for five minutes can speed healing significantly, that hospital gardens are especially effective for calming stressed patients, family members, and staff, and that patient exposure to nature reduces health-care costs.[i]
But scientific facts don’t tell the whole story. The personal testimonials posted at saveprouty.org offer compelling evidence of the difference that Prouty Garden has made. Shelley Senai tells what happened after her daughter Juniper was born with protruding bowels: “All told, we spent 101 days living at your hospital during the summer of 2013 and I can’t think of a day that we didn’t spend in the garden, unless it was raining….We met other parents there and got a feel for the community that was happening in this big hospital around us.” Caitlyn O’Hara, a lifelong cystic fibrosis patient who has relied on Prouty Garden for three decades and is waiting for a lung transplant, says pocket gardens and roof gardens do not compare: “A manufactured rooftop garden, no matter how lovely, cannot replace the magic of the natural world.”
More than 11,000 patients, families, staff, donors and community members have signed a change.org petition to preserve Prouty Garden. While they recognize the need for the proposed new hospital facilities, they argue that the garden, which is no less essential to its patients, patient families, nurses, physicians and other medical personnel, can and should be saved. Prouty Garden advocates are raising funds to press their case in ways that the board cannot ignore.
In New York City, trustees of the Frick Collection, a private art museum, recently decided to rethink expansion plans that would have eliminated the museum’s beloved garden for needed building space. If people were up in arms about the loss of a museum garden, how much more compelling and deep are the feelings evoked by the imminent loss of a hospital garden for sick and ill children.
I urge the hospital administration to declare a moratorium and go back to the drawing board. Surely, talented architects can produce a plan that avoids substantially altering the outdoor space that has been indispensable for the past six decades. Prouty Garden, which was intended to last forever, is about to be lost forever, unless the board changes course.
Thomas M. Paine, a landscape architect, is the author of Cities with Heart, about the importance of public open space. In 1976, he designed a corner of the Prouty Garden when he was an associate at Shurcliff, Merrill & Footit. He was a patient at the hospital in 1952.
Boston's Children's Hospital buying metro NYC physician group
http://cmg625.com/boston-childrens-hospital-buying-n-y-physician-group/